“This is the first hospital I’ve been to that has welcomed me like this.”
Your support will help patients like Enoc access dignified care for tuberculosis and other infectious diseases.

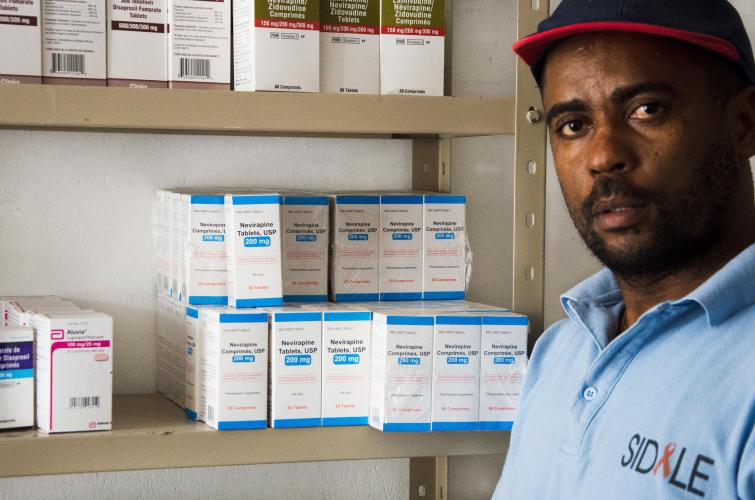
HIV in Haiti
First discovered in 1981, HIV quickly became a worldwide epidemic as globalizing forces enabled its spread across the land and between continents. Millions of people fell ill from this fatal disease and developed AIDS, which crippled their immune systems and allowed co-infections of tuberculosis and other diseases. Fear and stigma followed shortly behind as incomplete knowledge about HIV spread. It was hastily determined that Haitians, gay men, hemophiliacs, and heroin users were the four most likely populations to spread the epidemic. This stigmatization was solidified by the widespread adoption of the moniker “the 4H disease,” not accounting for the fact that people of all demographics were suffering from HIV.

Though Haitians were unjustly thrust into the spotlight as one of the four “most dangerous” populations, HIV had already begun to take a more morbid and immediate toll on the residents of this mountainous island. Amidst the economic effects of HIV stigma, namely a marked decline in the tourism industry, the virus was reaching those in even the most remote communities nestled in the southern regions of the island. By the mid-1990s, about one in every twelve of these Haitians were HIV-positive.
Haitians died from HIV and co-infections at terrifying rates throughout the late 1980s and 1990s. Nevertheless, it was said time and time again that HIV treatment in resource-poor settings like Haiti and sub-Saharan Africa was unfeasible. The barriers were monumental partly because of exorbitant drug pricing and partly because many believed indigent adherence to a daily HIV medication to be impossible. In fact, in 2001 the head of the U.S. Agency for International Development overtly declared this to the U.S. Congress by saying about Africans, “They do not know what watches and clocks are. They do not use Western means for telling time.”
Treatment Against The Odds
It wasn’t until local sister NGOs Partners in Health and Zanmi Lasante began providing anti-retroviral therapy (ARV) in 1998 through the HIV Equity Initiative that HIV-positive Haitians received the treatment that they needed and deserved. Shortly thereafter, the international community began a concerted push for more affordable and accessible ARV drugs, arguing that HIV could be treated in the furthest and most inaccessible corners of the world.
These concerted international efforts gave rise to the President’s Emergency Plan for AIDS Relief (PEPFAR) in 2003. With an original commitment of $15 billion to treat HIV/AIDS over five years, PEPFAR is perhaps the most significant investment in global health by any presidential administration. By implementing measures of prevention and providing ARV’s for treatment, this program has saved millions of lives from Vietnam to South Africa to Fond-des-Blancs, Haiti.
HEI/SBH and SIDALE
The community of Fond des Blancs has benefitted greatly from PEPFAR, which allows the CDC to fund SIDALE, the HIV/AIDS treatment and prevention program at HEI/SBH. SIDALE combines SIDA, the French acronym for AIDS, and “ale,” the French/Haitian Creole word for “go.” As its name suggests, the program has made landmark progress in reducing HIV transmission and managing the health of HIV-positive patients. HIV in Fond des Blancs was once considered a death sentence. Now, it has been reduced to a chronic, controllable disease.
SIDALE began in 2004 and was one of the first HIV/AIDS testing and treatment programs on Haiti’s Southern Peninsula. Before HEI/SBH’s partnership with the CDC and the Haitian Ministry of Public Health (MSPP), we could only test for HIV and provide mother-to-child prophylaxis. Long-term ARV treatment wasn’t possible. However, shortly after the advent of our original HIV program, PEPFAR allowed us to begin providing ARV treatment to HIV-positive patients. Since then, SIDALE has expanded to one of the most comprehensive and longitudinal care programs offered at SBH.
René, the HEI/SBH SIDALE Assistant Coordinator who has worked with the program since 2006, explains the reach of the program, “We currently have between 450 and 500 patients on HAART (Highly Active Antiretroviral Therapy) and about 1500 on palliative care. They come from as far as Port-a-Prince and Les Cayes for check-ups and medication.” He continues, “SIDALE is integrated throughout the entire hospital. Our HIV tests are administered by hospital nurses, our community awareness and education activities are done by community health nurses, and we have a strategy team that coordinates it all.”
The reach and effectiveness of HIV treatment programs in rural southern Haiti have far exceeded the low expectations of the late 1990s. With a population similar to those described as being incapable of following a daily regimen of medication, SIDALE has managed to ensure high rates of compliance through monthly ARV tracking and testing for controlled levels of CD4 cell counts, which can indicate good adherence to the regimen. Patients return to refill medication periodically and community health workers deliver medication to those who aren’t able to travel to the hospital. Contrary to the once-popular opinion, cultural barriers were not impossible to overcome.
Continuing Progress in HIV Treatment
René speaks with great pride about the changes he has seen over the past ten years. “People are sick and we help them get better. But, HIV treatment positively affects the social, economic, and psychological parts of life, too. For example, families with an infirm HIV-positive parent often couldn’t afford to send their children to school. Parents enrolled in SIDALE are able to return to work and send their children to school, which has many positive long-term effects.” He continues, “There has been a huge change in perception of HIV. In 2004, people in Fond des Blancs were scared to live with HIV. In 2014, they aren’t scared anymore. The community doesn’t stigmatize HIV-positive patients like they did in the past.”
Though great progress has been made to control HIV in rural southern Haiti, it still affects a significant portion of the population. One out of every fifty Haitians is HIV-positive and 6,500 Haitians died last year due to AIDS. Front-line workers like René battle tirelessly to provide friends and neighbors with life-saving treatment. They hope that support will continue to grow for their cause so that they can stop HIV from affecting the lives of people they know and love.
Your support will help patients like Enoc access dignified care for tuberculosis and other infectious diseases.
